Best CBD Oil for Anxiety: How CBD Helps with Stress & Depression

We all experience anxiety at one point or another.
Roughly 40 million Americans are diagnosed with clinical anxiety disorders every year, and countless others experience some form of anxiety on a daily or weekly basis. This anxiety can take a toll on our lives — affecting our relationships, performance at work or school, and our overall health and wellbeing.
One of the most popular alternative support options among anxiety sufferers is cannabidiol (CBD) — a non-psychoactive cannabinoid found in the hemp plant. This compound works through two main systems to promote a feeling of calmness and relaxation.
In this article, we’ll explain how CBD is suggested to support anxiety, what the research says, and offer some of the best hemp oil options for anxiety.
| PRODUCT | DETAILS | |
|---|---|---|
|
Best Overall CBD Oil
|
Royal CBD – Full Spectrum CBD Oil
|
Click for Best Price |
|
Best Organic Formula
|
Gold Bee – Organic CBD Oil
|
Click for Best Price |
10 Best CBD Oils for Anxiety (Top Quality Brands of 2025)
- Best Overall Pick: Royal CBD
- Best Organic Formula: Gold Bee
- Runner Up: CBD Pure
- Good Customer Support: Hemp Bombs
- Veteran Brand: CBDistillery
- Most Socially Responsible: NuLeaf Naturals
The CBD market hasn’t yet matured — which means there are a ton of brands offering inferior quality products. They’re managing to remain in business on hype alone. As the market matures, these companies won’t last — leaving only the best brands in the wake.
At this early stage in the market, it’s important that customers understand how to spot a good CBD manufacturer, and which companies to avoid.
To make things easier for you, I’ve compiled a shortlist of the best CBD oils I’ve come across for anxiety. Let’s cover each one in more detail before we go on to discuss exactly how CBD is reported to help with anxiety.
1. Royal CBD

Get 15% off all Royal CBD products. Use code “CFAH” at checkout.
Technical Details:
| Total CBD Content | 250 – 2500 mg |
| Available Flavors | Berry, Vanilla, Mint, Natural |
| Potency | 8.3 – 83.3 mg/mL |
What We Like About Royal CBD Oil:
Royal CBD is a California-based CBD brand with a growing collection of reviews from both regular users and industry experts.
Unlike many of its competitors, Royal CBD doesn’t rely on far-fetched claims in their marketing. The company also doesn’t specialize in gimmicky product types like we’ve seen from numerous other brands recently. The Royal CBD assortment is all about the classics. They keep it simple, focusing on full-spectrum CBD oil, THC-free CBD gummies, capsules, and CBD-infused topicals.
Royal CBD uses organically-grown hemp from the finest farms in California and Colorado. The company makes this CBD oil by first making a full-spectrum hemp extract using supercritical CO2. The extract is then dissolved in high-grade MCT oil and some flavorings to make the oil more enjoyable to use.
This CBD oil comes in 250 mg, 500 mg, 1000 mg, and 2500 mg – with the option of berry, mint, or other natural flavors.
I personally use Royal CBD’s 1000 mg full-spectrum CBD oil for my general anxiety disorder (GAD) & social anxiety. I should note that I tried 27 other brands before finding the one I liked!
With a 90-day, no-questions money-back guarantee – the only thing you have to lose your anxiety.
| Pros | Cons |
|
|
2. Gold Bee – Best Organic Formula

Technical Details:
| Total CBD Content | 1200 mg |
| Available Flavors | Natural, Kiwi-Honey |
| Potency | 40 mg/mL |
Gold Bee specializes in full-spectrum CBD oil that combines organic hemp with honey sourced from the Brazillian Rainforest. If not for the lack of high-potency oils, we would place this brand on the very top of our ranking due to the quality of ingredients it offers.
The full-spectrum extract is suspended in hemp seed oil to boost its bioavailability and keep everything in the cannabis family. Every product from Gold Bee’s line up is rigorously tested in third-party laboratories for their CBD content and purity. Unlike competitor brands, Gold Bee doesn’t use artificial flavorings and sweeteners in its products. The kiwi version of the oil is flavored with the said honey.
I use CBD oils for my morning anxiety when I can’t get my mind wrapped around my daily duties, and I’ve never been calmer since then. The 1200 mg potency also provides a nice dose of CBD before bed; I take it to unwind after spending most of the day in front of a computer screen, and I noticed a big difference in how rested I wake up the next day.
| Pros | Cons |
|
|
3. CBDPure (Runner Up)
Technical Details:
| Total CBD Content | 100 – 600 mg |
| Available Flavors | None |
| Potency | 20 mg/mL |
What We Like About CBDPure CBD Oil:
Similar to the other brands in our ranking, CBDPure sells full-spectrum CBD oil that has been sourced from domestically grown hemp and extracted with supercritical CO2.
If you’re looking for the highest potency, though, you might end up a little bit disappointed, as the maximum strength offered by their products is 600 mg of CBD per bottle, which is equal to 20 mg of CBD per mL. Our first choice, Royal CBD, has 30% higher potency than the strongest option available for this brand.
The good news is that these are full-spectrum extracts, so you need less CBD to find relief from anxiety than you would with CBD isolate. Each batch of CBDPure products is tested in a certified laboratory for the entire cannabinoid profile, terpenes, and flavonoids, as well as for potential contaminants.
If you’re not satisfied with this CBD oil for your anxiety, CBDPure has a 100% Satisfaction Guaranteed program, which allows you to get a full refund if you send the order back within 90 days after the purchase.
| Pros | Cons |
|
|
4. Hemp Bombs

Technical Details:
| Total CBD Content | 300 – 4000 mg |
| Available Flavors | Peppermint & watermelon |
| Potency | 10 – 133.3 mg/mL |
What We Like About Hemp Bombs CBD Oil:
Hemp Bombs is an American company specializing in the production of 99% pure CBD isolates. These products are available as standard tinctures, vape oils, capsules, or gummies.
Hemp Bombs CBD oil comes in five different potency options ranging from 300 mg to as much as 4000 mg of CBD per bottle. The CBD has been sourced from certified organic hemp plants from Europe and extracted with supercritical CO2 for the highest purity level.
This CBD oil option is made from CBD isolate — which means there’s nothing but pure CBD inside this oil. No THC or other cannabinoids, terpenes, or any other phytochemicals from the hemp plant. This offers a big advantage in that there’s guaranteed to be no THC in the bottle.
Isolate-based CBD oils are very versatile — you use them on their own, make DIY CBD infusions (e.g. creams and balms), add it to E-liquid for an extra punch, or use it in cooking delicious food. They’re also preferred for people who are using CBD alongside other supplements because there are fewer compounds that can potentially interact with the other health supplements.
Keep in mind that CBD isolate is purged from any cannabinoids other than CBD — so if you’re looking to take advantage of the entourage effect, you’re better off going for a full-spectrum CBD oil such as Royal CBD.
| Pros | Cons |
|
|
5. CBDistillery

Technical Details:
| Total CBD Content | 250 – 5000 mg |
| Available Flavors | Unflavored |
| Potency | 8.3 – 166 mg/mL |
What We Like About CBDistillery CBD Oil:
CBDistillery is an industry veteran, but make no mistake, the brand hasn’t rested on its laurels. On the contrary, CBDistillery continues to set high standards for its competitors, both in terms of the quality of ingredients and the potency of its products.
CBDistillery’s CBD oil is available in five different potencies, starting from 250 mg up to 5000 mg of full-spectrum CBD. The 2500 mg and 5000 mg options come in 30 mL bottles, which breaks down to 83–166 mg per serving — that’s enough CBD to keep you supplied for weeks or months.
What I love about CBDistillery’s assortment is that its products are sold at very reasonable prices. The 250 mg CBD oil costs around $20, so you don’t have to break the bank to get yourself a high-quality health supplement.
Users can choose between full-spectrum CBD oil and THC-free (broad-spectrum) oil, which is a nice move towards those who want to keep any traces of THC away from their system without losing the benefits offered by the entourage effect.
| Pros | Cons |
|
|
6. NuLeaf Naturals

Technical Details:
| Total CBD Content | 240 – 4850 mg |
| Available Flavors | Unflavored |
| Potency | 48 mg/mL |
What We Like About NuLeaf Naturals CBD Oil:
NuLeaf Naturals is another veteran brand that’s been selling CBD oil for over 5 years now. While they don’t have the broadest range of CBD products — only oil drops for humans and pets — this company definitely knows how to make an all-natural CBD oil.
All Nuleaf Naturals oils are sourced from domestic hemp and extracted with CO2. NuLeaf Naturals CBD oil has a beautiful amber-gold color, which is a good indicator of its quality. The oil is then filtered to remove any remaining plant matter.
NuLeaf sells its products in five different volumes — all in the same potency of 48 mg.mL CBD:
- 5 mL — 240 mg of CBD total
- 15 mL — 725 mg of CBD total
- 30 mL — 1450 mg of CBD total
- 50 mL — 2425 mg of CBD total
- 100 mL — 4850 mg of CBD total
| Pros | Cons |
|
|
7. Charlotte’s Web

Technical Details
| Total CBD Content | 200 – 1800 mg |
| Available Flavors | Mint Chocolate, Lemon Twist, Orange Blossom, Olive Oil |
| Potency | 7 – 60 mg/mL |
About Charlotte’s Web:
Charlotte’s Web is one of the oldest CBD companies in the United States. Founded by the Stanley Brothers, the brand has earned its reputation for helping now late Charlotte Figi with her intractable epilepsy. Despite several controversies about the health claims they made in the past, Charlotte’s Web didn’t lower its standards and still produce some of the best hemp extracts on the market.
Charlotte’s Web CBD oil is available in several concentrations: 200 mg, 500 mg, 1500 mg, and 1800 mg of total CBD. The highest potency provides 60 mg of full-spectrum CBD in every milliliter. You can choose between two bottle sizes (30 mL and 100 mL); Charlotte’s Web also offers flavored versions of its CBD oil, such as Mint Chocolate, Lemon Twist, Orange Blossom, and Olive Oil.
The company uses ethanol for extraction instead of the standard CO2 technology, which may leave a distinct aftertaste upon swallowing.
Pros:
- One of the most reputable brands on the market
- Full-spectrum CBD
- Delicious flavored versions
- Up to 1800 mg of CBD per bottle
- Available in two sizes: 30 mL and 100 mL
- Third-party tested for potency and purity
Cons:
- Non-organic hemp
- Ethanol extraction
- Suspension in olive oil (bitter taste)
- The company received a warning letter from the FDA in the past due to inappropriate health claims
8. cbdMD

Technical Details
| Total CBD Content | 300 – 7500 mg |
| Available Flavors | Natural, Berry, Orange, Mint |
| Potency | 10 – 250 mg/mL |
About cbdMD:
cbdMD is a North Carolina-based company that offers a wide range of CBD products, including tinctures, gummies, capsules, topicals, bath bombs, sleep aids, and pet products.
The company boasts a broad selection of pure CBD oils. The potency of these extracts ranges between 300 and 7500 mg of CBD per bottle; the highest concentration packs a healthy dose of 200 mg of pure CBD isolate suspended in MCT oil for improved absorption. cbdMD also offers four flavor options: natural, berry, orange, and mint.
On the one hand, it could be challenging to find another company with such concentrated products; but on the other hand, these CBD oils are based on a broad-spectrum extract, which doesn’t evoke the full entourage effect. Therefore, higher potency may not translate into better results.
Transparency-wise, cbdMD provides up-to-date certificates of analysis from a third-party laboratory. They are available on the company’s website; you can find them by entering the product’s batch.
Pros:
- US-grown, non-GMO hemp
- CO2 extraction
- THC-free
- Up to 7500 mg of CBD per bottle
- Batch-specific certificates of analysis
Cons:
- Limited entourage effect due to the lack of THC
- Most people don’t need such high doses of CBD in their routine
9. Medterra

Technical Details
| Total CBD Content | 500 – 3000 mg |
| Available Flavors | Natural, Citrus, Mint Chocolate |
| Potency | 16 – 100 mg/mL |
About Medterra:
Medterra is a small California-based company that offers premium CBD extracts in different spectra: full-spectrum, broad-spectrum, and isolates. The potency of these oils ranges between 500 mg and 3000 mg of CBD per bottle, which is a standard range. Aside from the unflavored version, there are two flavored options: Citrus and Mint Chocolate.
The full-spectrum CBD oil is also infused with 2 mg of THC per bottle, which the company claims to be the true full spectrum of cannabinoids. However, the problem with this version of Medterra’s CBD oil is that they aren’t legal in all 50 states because they contain more than 0.3% of THC.
So, if you want to buy Medterra’s products in all 50 states, your options are limited to broad-spectrum extracts and isolates. These come in higher potencies, upwards of 1000 mg of CBD per bottle.
All of Medterra’s CBD oils are tested in a third-party laboratory for potency and purity, including the results for pesticides, heavy metals, and residual solvents.
Pros:
- Premium-grade CBD oils
- Up to 3000 mg of CBD per bottle
- Available as full-spectrum CBD, broad-spectrum CBD, and isolates
- Lab tested for potency and purity
Cons:
- The “real” full-spectrum CBD oil isn’t available in all states
- Some of the lab reports indicate higher CBD levels than stated on the bottle
- No discounts for returning customers
10. Joy Organics

Technical Details
| Total CBD Content | 450 – 900 mg |
| Available Flavors | Tranquil Mint, Fresh Lime, Summer Lemon |
| Potency | 15 – 30 mg/mL |
About Joy Organics:
Joy Organics is one of the most reputable CBD vendors in this space. The brand was founded by a woman named Joy Smith, who has been exploring the benefits of CBD oil for her problems with pain and sleep.
Joy Organics offers a range of broad-spectrum CBD extracts sourced from certified organic hemp. The company has plenty of positive reviews all over the internet. They also haven’t received any warning letters from the FDA yet.
The Joy Organics CBD oil is formulated with broad-spectrum CBD in a modest potency range, from 450 to 900 mg of CBD per bottle. These oils are available in three refreshing flavors: Tranquil Mint, Fresh Lime, and Summer Lemon. The highest potency provides 30 mg of CBD in every milliliter, which is a standard dose for most people in terms of daily supplementation.
In 2018, one of the company’s citrus tincture was found to contain a fungicide that is commonly used on citrus fruit during independent testing. Fortunately, Joy Organics recalled the product immediately following this and implemented a new third-party testing system.
Pros:
- Non-GMO, US-grown hemp
- Supercritical CO2 extraction
- Broad-spectrum CBD
- THC-free
- Delicious flavors
Cons:
- A bit expensive
- No high-strength oils
What is CBD Oil?
CBD, short for cannabidiol, is one of the active ingredients in the cannabis plant (Cannabis sativa). This includes both industrial hemp plants, and marijuana.
CBD is the modulator to the endocannabinoid system — a complex neurochemical network responsible for controlling various vital functions in the human body and brain. The endocannabinoid system regulates processes such as:
- Memory
- Cognitive performance
- Body temperature
- Sleep regulation
- Immune function
- Pain perception
- Reproduction and fertility
- Mood and emotion
- Hunger and satiety
CBD helps the endocannabinoid system maintain chemical balance within the body — also known as “homeostasis” or “equilibrium.” If homeostasis isn’t maintained, we become sick. Depending on which aspect of homeostasis is out of balance — the effects on the body will be very different. If our nervous system is affected, it can lead to symptoms of anxiety, stress, and emotional instability.
CBD has other effects on the body as well — the most relevant in the context of this article are its effects on a neurotransmitter called GABA — which is responsible for slowing us down when we become overstimulated. We’ll get into how this works in more detail later.
There are many different ways to use CBD — it’s added to capsules, infused in topical salves and creams, mixed into gummy candies, and added to vape oils. But by far the most popular form of the supplement is in the form of an oil. CBD oils are made by mixing the fat-soluble hemp extracts rich in CBD and other cannabinoids with an oil base — in most cases MCT oil or hemp seed oil.
Using CBD in the form of oil makes it easier to measure doses since you simply have to count the number of drops or measure the oil with the built-in dropper. Compare this to pure hemp extracts which require scales and a lot of experience to accurately measure the right dose.
Additionally, the oil content of CBD oils significantly improves the absorption rate in the digestive tract. This helps make the CBD more efficient — allowing you to use less CBD for the same level of benefits.
What Causes Anxiety?

Anxiety is defined as “an emotion characterized by feelings of tension, worried thoughts, and physical changes like increased blood pressure.” It’s a natural process developed over the course of human evolution to protect us from environmental threats like changes in our environment, exposure to predators, or other dangers. Feeling anxious helps us identify and avoid dangers that pose a threat to our health and wellbeing.
Anxiety can also become pathological — leading us to feel excessive stress and worry in situations that are not life-threatening. Modern stresses like work deadlines, relationship problems, or social expectations can all cause us to feel anxious. If this happens too often or in excessive amounts, it can cause us more harm than good.
There are many forms and levels of intensity of anxiety symptoms — including generalized anxiety disorder, panic disorder, post-traumatic stress disorder, social anxiety, insomnia, and many different phobias.
It’s wise to speak with your doctor if you experience severe anxiety attacks, or if your anxiety begins affecting your ability to live your life. There are many underlying causes for anxiety, so it’s best if a medical professional can explore some of these options to help you find the best form of treatment.
Why Are Pharmaceutical Anxiety Medications Dangerous To Our Health?
The most common form of drug treatment for anxiety is a class known as benzodiazepines. These medications bind to the GABA receptors in the brain to force electrical activity to slow down — thus alleviating the most common signs of anxiety. This works in a similar way to CBD, but is significantly stronger and more specific.
The main problem with conventional anti-anxiety medications is that they can become highly addictive — often leading to a worsening of symptoms over time as tolerance to the medications begins to form.
Here’s the problem…
You take benzodiazepines to fight anxiety and for a time it works. However, the body quickly forms a tolerance to the medication to resist its effects by removing some of the GABA receptors. Once these receptors are gone, we need more of the medication to produce the same effect. This process continues until we’ve reached the maximum dose for the drug. If the drug starts to wear off, we no longer have enough GABA receptor activity to keep our nervous system from going into hyperdrive — forcing us into a state of extreme anxiety.
The body will eventually reach a point where we require the drug just to not have an anxiety attack.
Benzodiazepines aren’t the only option, but they’re the most common. Other classes of medications used for treating anxiety have similar effects long-term.
Some examples of anti-anxiety medications include:
- Benzodiazepines
- Barbiturates
- Opioids
- SSRIs
- Tricyclic antidepressants
Side-effects to these medications are common and can range in severity. Most of the drug classes on the list will cause tolerance in the body, as described above.
Here are some of the most severe side effects of prescription anti-anxiety medications:
- Nausea
- Insomnia
- Agitation
- Irritability
- Constipation
- Arrhythmia
- Galactorrhoea
- Cardiac disease
- Blurred vision
- Collapse
- Weight gain
With all these negatives, it’s no wonder why CBD has become such a popular alternative treatment option for anxiety and related conditions. You can check our post to know more about the risk of taking CBD with Xanax — a prescription drug that belongs to benzodiazepines medications.
Potential Benefits of CBD Oil For Anxiety
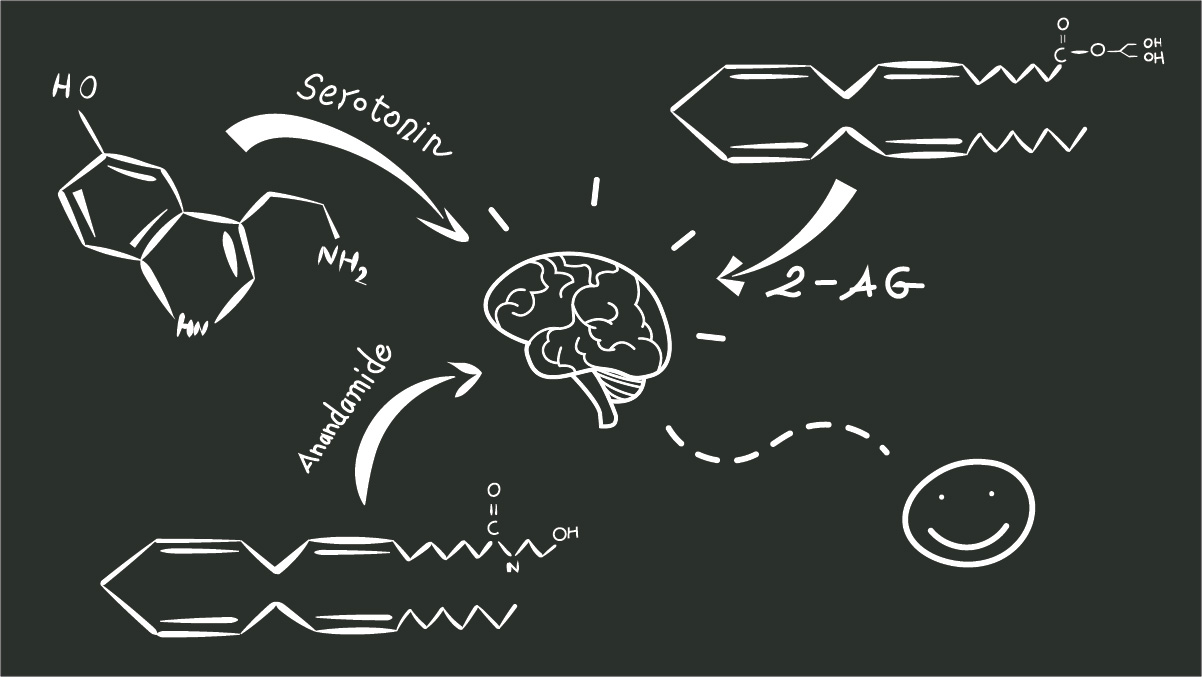
At the very beginning of the article, we mentioned that the endocannabinoid system regulates our response to fear, among many other functions.
Unlike conventional anti-anxiety treatments, CBD oil doesn’t just mitigate the symptoms of anxiety — it gets down to the root of the problem by regulating endocrine disruptions as well as the amount of anandamide in our brains — a compound aptly named the “bliss molecule.”
CBD has been shown to help with anxiety in a few different ways. While the majority of research describing how CBD works for this disorder is either preclinical or based on animal studies, there are hundreds (if not thousands) of testimonies from people who have found relief in CBD oil after failing with the conventional treatment. There are also a handful of randomized, double-blind, clinical trials conducted on the interaction as well. These are considered to be the highest form of clinical research available.
Let’s cover the mechanisms of action CBD oil uses to support anxiety levels and what the research says about this incredibly useful molecule.
1. Serotonin Receptors & Brain Activity
CBD has been shown to stimulate the 5HT1 serotonin receptors. In simple terms, this cannabinoid increases serotonin activity in the brain — which affects the transmission of electrical activity as well as mood, concentration, and sleep.
Studies have shown a direct link between the activity of serotonin as the 5HT1 and 5HT2 serotonin receptors in the central nervous system and anxiety disorders.
2. Anandamide Production — The Bliss Molecule
The next anti-anxiety effect of CBD is linked to its ability to increase the amount of the body’s natural endocannabinoids — anandamide and 2-AG. This effect is particularly prominent for anandamide in particular.
Anandamide has almost the same chemical structure as THC, the cannabinoid responsible for triggering euphoric and psychoactive effects in cannabis users.
Anandamide doesn’t cause psychoactive effects like THC, but it is closely correlated with feelings of bliss, joy, and euphoria. In contrast, lower anandamide levels are thought to result in a low mood or “overreaction” to stress and anxiety triggers.
CBD has been shown to enhance the activity of anandamide by preventing its breakdown and metabolism — ultimately leading to elevated levels of the bliss molecule in the brain.
3. Hippocampal Neurogenesis — Homeostasis & Anxiety
The hippocampus is a critical brain region tasked with controlling homeostasis in both the brain and body.
Brains scans of patients struggling with anxiety and depression often exhibit changes in the hippocampus, and successful anxiety treatment is associated with the production of new neurons (neurogenesis) in this area. Some research has shown.
It appears that CBD may stimulate the hippocampus to regenerate neurons, which could be groundbreaking for anxiety patients (5).
Current evidence suggests that severely damaged neuronal plasticity may influence suicidal behavior — so, regenerating neurons in the hippocampus is thought to reduce the chances of depressive behavior.
4. GABA Receptors — The Brake Pedals for the Brain
Earlier, we spoke about the interaction CBD has with our GABA receptors. Let’s dig into this a little more and discuss exactly how this works and how it relates to anxiety.
GABA essentially acts as the brake pedal for the nervous system. It’s used to keep our speed in check when we become agitated. If GABA isn’t doing its job effectively, we can quickly begin to speed out of control — resulting in symptoms commonly referred to as anxiety.
CBD binds to the GABA receptors in the nerve cells and makes them more sensitive to GABA. This would be like changing the brake pads on your car, so you don’t have to hit the pedal as hard to begin slowing down.
Research has shown that insufficient GABA activity is closely involved in the development of anxiety disorders. CBD has been shown to interact with the GABAa receptors in the neurons, offering a precise mechanism for its anti-anxiety benefits. Other cannabinoids in the cannabis plant have also been shown to support this process through GABA and other chemical pathways in the brain.
The Best CBD Oil For Anxiety: What to Look For

The hemp industry has proven to be a lucrative market for many companies. Still, as with so many emerging businesses, it’s a tantalizing sector for sketchy companies trying to cash in on unaware customers.
You want to steer clear of inferior CBD supplements as much as possible. Such products are often made from low-quality hemp, extracted with toxic solvents, and promise a lot more than CBD oil is capable of.
When searching for the best CBD products for anxiety online or in local stores near you, keep an eye out for the following details:
1. Hemp Source — Opt For Domestic
Hemp is an effective bio-accumulator, meaning it absorbs everything from the soil it grows in. When grown in polluted soil, the plant may accumulate heavy metals and other harmful toxins, resulting in a poor end product. Hemp grown in places like China or India is especially high in these toxic elements because of high soil contamination in the region.
If you want a high-quality CBD oil to help you deal with anxiety, look for products that have been sourced from domestically grown hemp. US farmers are subject to strict quality control standards, and the growing competition prevents them from cutting corners in their cultivation practices.
Plus, many US growers use organic growing methods even if their CBD oil is not certified organic, mainly due to the high cost of these certifications. Always ask your potential vendor how they source their plants to ensure you’re not throwing your money down the drain.
2. Extraction Method — Look For CO2 Extraction
The majority of high-quality CBD oils are extracted with supercritical carbon dioxide. This method produces a pure and highly potent product, leaving you with pure extracts free of any toxic solvent residue.
CBD tinctures, which are a bit different than CBD oil, are extracted with high-proof alcohol. Some less common extraction methods call for using olive oil, but when a company isn’t open about how it obtains its CBD extracts, that should raise a red flag because that means they probably applied some toxic solvents in the process. And what’s worse, there’s a risk these solvents weren’t completely removed after extraction.
3. Full-Spectrum Hemp vs. CBD Isolate
What do you want to achieve with your CBD oil aside from anxiety relief?
Are you aiming at maximizing your CBD dose per serving?
Or is the whole-plant synergy more important than the potency of cannabidiol?
If you want a versatile product and high doses of CBD — isolate-based CBD oil will be your best bet. On the other hand, full-spectrum extracts offer one perk that isolates users cannot achieve with their products — the entourage effect.
The entourage effect refers to the synergistic effect achieved by all active compounds in cannabis plants. Researchers suggest each of these compounds work in unison to amplify the benefits of one another, resulting in a greater therapeutic potential.
The cannabis community appears to support this concept; the Internet is full of testimonies from people who switched from isolates to full-spectrum CBD oil for anxiety because they needed lower doses to get relief.
4. Additional Ingredients
High-quality CBD oil contains two main ingredients — CBD extract and carrier oil in which the CBD is dissolved.
Additionally, CBD oil can have some natural flavorings added to mask the hemp aftertaste. Some products are infused with supplementary herbs and organic compounds to amplify the stress-relieving properties of cannabidiol — such as chamomile or melatonin.
In general, a complex formula involving hemp extract and other herbs and nutrients formulated for a specific application is going to be better overall.
5. Laboratory Testing Results
3rd-party lab testing is the ultimate way to verify the credibility of your CBD vendor.
Not only do such tests check for the potency of CBD in the final product, but they also list the entire cannabinoid profile and can detect any impurities that could compromise its quality.
If the brand actually uses premium ingredients in its CBD oil (as they claim), they should be open about their lab testing reports and list the results publicly on the company website. If these tests aren’t available, we suggest you move on to look elsewhere for a company that does this.
CBD Oil For Anxiety: Key Takeaways
As scientists conduct more research on the health benefits of CBD, we’re beginning to unlock new applications of this incredible plant-extract. One of the hottest areas in research at the moment is for the use of CBD with anxiety.
CBD oil works by interacting with the endocannabinoid to support homeostasis (balance), modulate GABA activity, and support serotonin and anandamide levels — all of which play a key role in the process of stress and anxiety.
The greatest challenge lies in finding the best CBD oil for anxiety out of the sea of fly-by-night CBD brands. As long as you know what characteristics make for an excellent CBD brand and what the red flags are for scam or poor-quality products — you should be able to find a product that suits your individual needs.
If you’re not sure where to start, I highly recommend you go with Royal CBD as your CBD oil of choice. The 1000 mg option offers the best value for money, and high-grade full-spectrum extract has served me well with my anxiety in the past.
Have you tried using CBD for anxiety? How did it work for you? Let us know in the comments!
References:
- Beesdo, K., Knappe, S., & Pine, D. S. (2009). Anxiety and anxiety disorders in children and adolescents: developmental issues and implications for DSM-V. The Psychiatric clinics of North America, 32(3), 483–524.
- Blessing, E. M., Steenkamp, M. M., Manzanares, J., & Marmar, C. R. (2015). Cannabidiol as a Potential Treatment for Anxiety Disorders. Neurotherapeutics: the journal of the American Society for Experimental NeuroTherapeutics, 12(4), 825–836.
- Russo, E.B., Burnett, A., Hall, B., and Parker, K.K. (2005). Agonistic Properties of Cannabidiol at 5-HT1a Receptors. Neurochemical Research, 30(8), 1037-1043.
- Leweke, F. M., Piomelli, D., Pahlisch, F., Muhl, D., Gerth, C. W., Hoyer, C., … Koethe, D. (2012). Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia. Translational psychiatry, 2(3), e94.
- Beale, C., Broyd, S. J., Chye, Y., Suo, C., Schira, M., Galettis, P., … Solowij, N. (2018). Prolonged Cannabidiol Treatment Effects on Hippocampal Subfield Volumes in Current Cannabis Users. Cannabis and cannabinoid research, 3(1), 94–107.
- Wenzel, A., Haugen, E. N., Jackson, L. C., & Brendle, J. R. (2005). Anxiety symptoms and disorders at eight weeks postpartum. Journal of anxiety disorders, 19(3), 295-311.
- Bakas, T., Van Nieuwenhuijzen, P. S., Devenish, S. O., McGregor, I. S., Arnold, J. C., & Chebib, M. (2017). The direct actions of cannabidiol and 2-arachidonoyl glycerol at GABAA receptors. Pharmacological research, 119, 358-370.
- A World Health Organizadon Demonstration Project. (1994). A phase II study of delta-9-tetrahydrocannabinol for appetite stimulation in cancer-associated anorexia. Journal of palliative care, 10(1), 14-18.
- Charney, D. S., Woods, S. W., Goodman, W. K., & Heninger, G. R. (1987). Serotonin function in anxiety. Psychopharmacology, 92(1), 14-24.
- Bannerman, D. M., Rawlins, J. N. P., McHugh, S. B., Deacon, R. M. J., Yee, B. K., Bast, T., … & Feldon, J. (2004). Regional dissociations within the hippocampus—memory and anxiety. Neuroscience & Biobehavioral Reviews, 28(3), 273-283.

